Translate this page into:
Overcoming diagnostic challenges of artificial intelligence in pathology and radiology: Innovative solutions and strategies
*Corresponding author: Rupali Gautam, Department of Pathology, Mangalam In Vitro Lab, Gandhidham, Kutch, Gujarat, India. rupaligautam9@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Shah RM, Gautam R. Overcoming diagnostic challenges of artificial intelligence in pathology and radiology: Innovative solutions and strategies. Indian J Med Sci 2023;75:107-13.
Abstract
The advent of artificial intelligence (AI) has brought about significant changes in the fields of pathology and radiology, particularly in the area of diagnostic accuracy. Although AI has enormous potential for enhancing the precision and effectiveness of diagnosis, it also presents an array of challenges. This review article examines the diagnostic challenges of AI in pathology and radiology. The article begins by giving a general review of AI and its potential applications in pathology and radiology. It then discusses the challenges posed by AI in the areas of data quality, generalization, interpretability, and hardware limitations. The article also explores the ethical and regulatory implications of AI in diagnostic settings, including issues of bias and transparency. Finally, the article offers potential solutions to address these challenges, such as standardization of AI algorithms, data sharing initiatives, saliency mapping, adversarial training of algorithms, cloud computing, edge computing, hybrid approaches, and increased collaboration between human experts and AI systems. Overall, this review highlights the critical importance of addressing the diagnostic challenges of AI in pathology and radiology to make sure AI is able to achieve its potential to enhance patient care.
Keywords
Artificial intelligence
Diagnostic challenges
Digital pathology
Digital radiology
Solutions
INTRODUCTION
The role of artificial intelligence (AI) in pathology and radiology is rapidly expanding and promises to revolutionize patient care in the coming years. Radiology was relatively quick to adopt AI whereas pathology (surgical pathology specifically) only recently began utilizing AI.[1]
Pathology and radiology form the core of cancer diagnosis.[2] Radiology locates unusual lesions and provides information on the clinical stage and any probable comorbidities linked with it, whereas pathology establishes particular histologic and molecular characteristics of tissues. Pathology and radiology form an innovative diagnostic tool, which, when combined with genetics, forms the integrated diagnosis. Demand for deep integrated workflows between radiology and pathology has recently increased, owing primarily to technological advances in computational sciences that enable meaningful integration of these diagnostic specialties.[3] Numerous studies have shown the importance of this integration in the context of a particular cancer diagnosis, where integration and correlation between the two specialties were shown to be able to identify misdiagnosis and to encourage repeat sampling in cases of unexplained discrepancy between imaging and pathologic findings.[4]
AI’s significant advances in digital radiology (DR) and digital pathology (DP) hold enormous potential. In the field of AI, significant development has occurred in studies that focus on the strategic aspects of challenges, acceptance, and consensus to advance and incorporate technology in the field of health.[5]
The routine use of AI in radiology and pathology workflows would undoubtedly result in significant benefits.[6] They range from reducing workload to instrumentation quality control (QC). The potential of feature recognition, automatic recognition, and QC, along with the drawbacks and associated issues, are of interest to these researchers.[7,8] Certainly, the evolution of digitalization processes in the DP world[6] is slower than in DR world, especially because DP has not adapted to the Digital Imaging and Communications in Medicine (DICOM) standard with the same readiness as the DR. Another factor is the “black box” nature of AI image models, which makes it difficult to comprehend why the algorithm makes certain predictions.[9]
The integration of AI in the health domain faces many ongoing challenges. To achieve a successful integration of AI with DR and DP, it is crucial to: (a) Create new challenges “separating Hope from Hype” and avoiding pitfalls (b) to make sure that insiders acceptance and agreement processes accompany these difficulties as these technologies will be used in their workflow.[10]
The application of AI to medical imaging, encompassing yet not confined to image processing and interpretation, constitutes one of the most potential areas of health-care innovation.[11] AI systems, in particular deep learning, have made great progress in image recognition and classification, offering excellent diagnostic accuracy for a variety of disorders.[12]
While AI has enormous potential; there are several challenges that must be overcome. The main diagnostic challenges of AI include lack of high-quality datasets, standardization, interpretability, bias, ethical and regulatory issues, hardware limitations, and cost.
This review article aims to explore the diverse applications of AI in pathology and radiology, along with an analysis of the challenges that this field is facing, and the potential solutions that can be implemented to address these challenges.
APPLICATIONS OF AI IN PATHOLOGY AND RADIOLOGY
AI is being used in radiology and pathology of chronic diseases like cancer to develop accurate and effective inventions that will help treat patients who have these diseases as well as ultimately find a cure for them.[13] AI algorithms can analyze large volumes of medical data, including medical images and patient records, to identify patterns and make predictions. The following constitute the primary categories of AI applications in pathology and radiology.
Diagnostic applications
Computer vision algorithms can extract multiple features from whole slide images (WSI) to make diagnostic predictions. One of the key advantages of AI in pathology is its ability to precisely evaluate quantitative features such as immunohistochemical biomarker assessment, cell counting, and various tissue features like cell arrangement, architecture, structure density, and distribution pattern.[14] AI algorithms can assist in standardizing histological scoring standards for morphological traits that reflect an array of cellular processes, like Gleason score for prostatic carcinoma and breast cancer grading.[15,16] AI helps in lymph node examination and metastasis detection. A deep neural network-based technique has been proven to be capable of classifying and categorizing hundreds of WSI from prostate cancer, basal cell carcinoma, and breast cancer metastases to axillary lymph nodes. As a result, the pathologists will be able to remove 65–75% of slides while maintaining 100% of sensitivity.[17] AI algorithms can accurately classify WSI of colorectal polyps such as hyperplastic, sessile serrated, tubular, and tubulovillous/villous polyps.[18]
In radiology, AI has numerous applications including computer-aided detection (CAD), computer-aided diagnosis (CADx), and image segmentation. CAD involves using AI algorithms to analyze medical images and detect abnormal features that may be indicative of disease. CADx uses AI algorithms to provide a step further and uses AI algorithms to provide a diagnosis based on reviewing of images. Image segmentation involves using AI algorithms to identify and label different parts of a medical image, such as organs, blood vessels, or tumors. This can help radiologists locate abnormalities more easily and accurately and aid in the planning of surgical procedures.
AI algorithms have been developed to identify potential abnormalities in medical images, such as X-rays, computed tomography (CT) scans, ultrasound scans, and magnetic resonance imaging scans. This can lead to faster and more accurate diagnosis, especially in cases where time is of the essence, such as in stroke or heart attack. These algorithms can assist radiologists in detecting cancer, identifying bone fractures, heart diseases, nodules and masses on X-rays, and detecting early signs of Alzheimer’s disease.
Predictive and prognostic analytics
AI algorithms can analyze patient data to predict the likelihood of certain medical conditions, such as cancer or cardiovascular diseases, enabling early intervention and treatment. On the basis of morphological characteristics, AI can prognosticate a patient’s outcome and responsiveness to a certain medication.[19]
Workflow optimization
AI can help automate and streamline many aspects of both pathology and radiology workflows, such as image analysis, report generation, and communication with other health-care professionals.
Quality Control
Although being a time-consuming stage in the diagnostic routes, ensuring the QC of slides is currently highly crucial. AI tools can detect a range of flaws in scanned slides such as staining quality, tissue representation, processing faults, tissue fixation quality, and staining quality of control samples.[20] In radiology, an amalgamation of machine learning, for natural language interface classification and deep learning (e.g., convolutional neural networks) models, has been studied in deciding on a suitable imaging study protocol based on the patient’s signs and symptoms and prior imaging reports, obviating the need for an experienced radiologist for the same.[21]
Treatment planning
AI algorithms can assist in treatment planning for certain medical conditions, such as cancer. By analyzing medical images and patient data, AI can help determine the most effective treatment options for individual patients.
DIAGNOSTIC CHALLENGES OF AI IN PATHOLOGY AND RADIOLOGY
Despite the potential benefits of AI in pathology and radiology, there are still several diagnostic challenges that need to be addressed before widespread adoption of these technologies can be realized [Figure 1].

- Challenges faced by artificial intelligence in pathology and radiology.
Lack of standardization
One of the main challenges of using AI is the lack of standardization in imaging and diagnostic protocols. This makes it difficult for AI algorithms to accurately analyze medical images and identify potential abnormalities. Each step of high-quality pathology slide preparation, including embedding, cutting, staining, and scanning, is critical to the successful adaption of WSI in DP. Folded tissue section during cutting, staining variation, and the presence of air bubble during covering slide as well as different settings of brightness, intensity disparity, and boundary intensity during scanning can cause unreliable raw data and produce inaccurate results.[22] A single noise in big data can cause misclassification and change the slide prediction, resulting in a large number of false positives or negatives.
Data quality is a major challenge in radiology. Medical data can be noisy, incomplete, and inconsistent, making it difficult for AI algorithms to learn accurately. Testing reproducibility of a proprietary algorithm can be very difficult in one single site; expanding the evaluation to other sites and different datasets can be extremely complex. This is especially true because machine learning applications do not always follow the same pipeline from data ingestion to output, and no standardization of the process exists.[23]
Generalization/Limited training data
There is a lack of training data that is high quality enough to make AI algorithms. There is also an issue of data being not large enough to cause development of good AI systems. Institutional xenophobia may restrict access to image data between institutions. Failure to assemble a sufficiently large enough training set is a potential pitfall that could have the effect of making the results less accurate or generalizable.[24]
Interpretability
While AI algorithms can make accurate predictions, it can be difficult to understand how they arrive at their conclusions. The inherent limits in distinguishing normal versus abnormal in continually variable biologic data may be the most significant limitation for AI in imaging.[25] This can make it challenging for clinicians to trust and interpret the results of AI models and can limit the use of AI in clinical decision-making.
Bias
AI algorithms can be biased and can reflect and reinforce existing biases in healthcare. This can lead to disparities in health-care outcomes for certain patient populations. Recent literature on medical data has shown algorithmic bias in demographic inequities.[26] Alleviating medical data bias can provide meaningful data normalization where patient data are being analyzed and not being inaccurately predicted.[27]
Regulatory and ethical considerations
The use of AI raises important regulatory and ethical considerations. For example, AI models may be subject to regulation by government agencies and to legal and ethical requirements related to privacy, data security, and informed consent. In addition, AI application in health-care raises important ethical considerations related to the impact on patient care, the role of clinicians in decision-making, and the potential for AI to replace healthcare workers.
Higher precision medicine can be made possible by constantly huge, sensitive health data transfer between hospitals and research facilities, but doing so also raises the risk of security breaches. It is difficult for computational pathology to obtain health databases because of laws enforcing stringent patient privacy protections; hence, larger training data sets are required.[28]
Future of Research Communications and e-Scholarship (FORCE11) advises adhering to the findable, accessible, interoperable, and reusable (FAIR) principles for shared data to maintain its value.[29] It is a set of principles and guidelines aimed at making data more discoverable, accessible, and reusable. In the context of AI, FAIR data sharing is crucial for ensuring that the data used to train and validate AI models are of high quality, can be easily accessed and understood, and can be used across different research projects or applications. If data are standardized from the beginning, adherence to these standards will be easy.
Findable: Data should have accurate and rich metadata, including standardized and unique identifiers, making it easy to locate and identify specific datasets.
Accessible: Data should be openly available or accessible under controlled conditions, taking into account privacy, legal, and ethical considerations.
Interoperable: Data should be structured using common standards, formats, and vocabularies, allowing seamless integration and exchange of data between different systems.
Reusable: Data should be well-documented, with clear usage licenses and permissions, enabling others to reuse the data for new analyses and research purposes.
Interoperability is hampered by the requirement for manual transformation and mapping in the absence of appropriate data exchange standards and domain-relevant content standards.[30] Common data elements (CDEs) have been used to standardize data collection. CDEs are standard data elements, definitions, and formats that are agreed on and used consistently across different research domains. They serve as building blocks for creating structured and standardized datasets, facilitating data integration, harmonization, and interoperability. CDEs play a critical role in AI applications that rely on large-scale data analysis.
By employing CDEs, researchers can easily share and combine data from multiple sources. This promotes consistency, comparability, and compatibility of the data collected and shared for AI analysis. It enhances the reliability and reproducibility of AI models, as well as facilitates collaboration and knowledge sharing among diverse research teams and institutions. With CDEs, AI-driven advancements in pathology, radiology, and other health-care domains can be achieved with greater accuracy and efficiency.
Together, FAIR data sharing and CDEs support the development and deployment of robust AI models in pathology, radiology, and other health-care domains.
Hardware limitations
One of the main hardware limitations of AI is processing power [Figure 2]. AI algorithms require large amounts of computational power to analyze medical images and identify potential abnormalities. This can be challenging for health-care facilities that may not have access to high-performance computing resources or for clinics and hospitals in remote or underserved areas where internet connectivity and power supply may be limited.
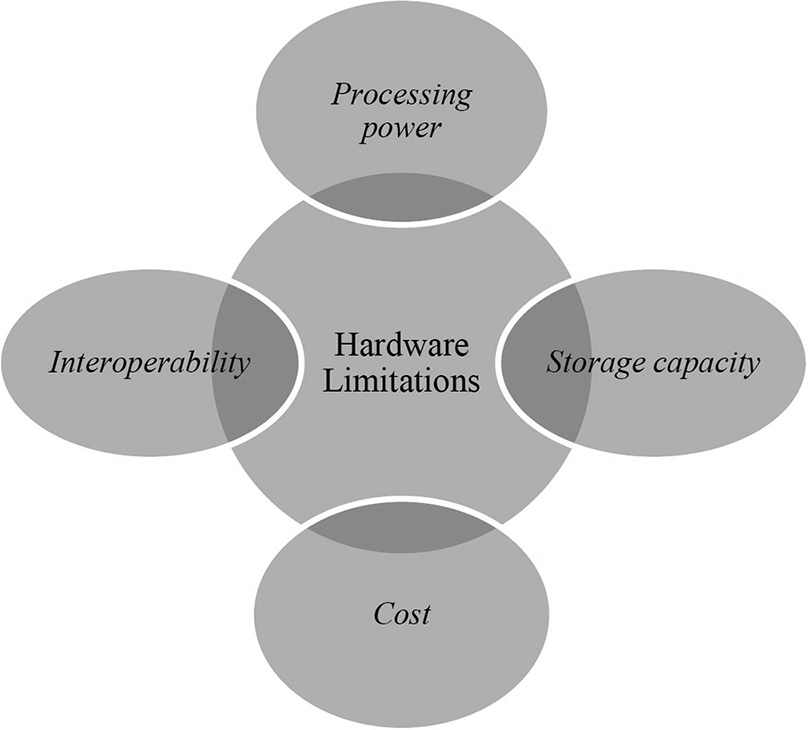
- Hardware limitations of artificial intelligence.
Another hardware limitation of AI in DR and pathology is storage capacity. Medical images can be large and complex, and AI algorithms require significant storage capacity to store and analyze these images. This can be a challenge for health-care facilities that may not have access to large-scale storage solutions or for hospitals in resource-constrained settings where storage capacity may be limited.
Interoperability is another hardware limitation. Different imaging modalities and diagnostic systems may use different hardware and software platforms, which can make it difficult to develop and deploy AI algorithms that work seamlessly across multiple systems. This can limit the applicability of AI in certain areas of medicine and can create challenges for health-care providers who may need to access and analyze medical images from multiple sources.
Finally, cost can be a significant hardware limitation of AI in DR and pathology. High-performance computing resources, storage solutions, and other hardware requirements for AI can be expensive and may be prohibitive for many health-care facilities and clinics. This can limit the adoption and deployment of AI in certain areas of medicine and can create disparities in access to AI-based diagnostic tools and technologies.
These are few of the key diagnostic challenges of AI in pathology and radiology. As researchers continue to develop and refine AI algorithms for medical imaging and diagnosis, it will be important to address these challenges to ensure that AI is used in a safe, effective, and ethical manner.
OVERCOMING AI’S LIMITATIONS
Despite the initial success of AI image models in pathology and radiology, their adoption in everyday practice has lagged behind expectations. Here are a few examples of how AI can be applied here:
Data quality
One of the biggest challenges in developing AI algorithms is ensuring that the data used to train these algorithms are of high quality. These issues can be resolved with the assistance of machine learning models and advanced algorithms, allowing for more accurate diagnosis and treatment recommendations. High-quality clinical data are crucial for conducting prospective, randomized, and multicenter trials required to find AI solutions, in addition to image data.[31]
Advanced solutions for data cleaning and validation can include techniques such as automated image segmentation, QC algorithms, and outlier detection. In addition, data enhancement techniques can be employed to produce additional training data and reduce the risk of overfitting. Standards for medical images in radiology and pathology were developed by the DICOM initiative. It specifies medical image exchange protocols which support the data and quality requirements for clinical application. By introducing a method for dealing with tiled big images as multi-frame images and numerous images at different resolutions, DICOM standard now offers WSI functionality.[32]
Many researchers are exploring collaborative data sharing projects, where large-scale datasets are shared and merged across various institutions or nations. For example, a medical image repository with free access, known as the cancer imaging archive, enables researchers to access and analyze large amounts of high-quality imaging data for cancer research.
Generalization
One possible solution to this challenge is to use a diverse training dataset that includes a wide range of cases. For example, if an AI model is being trained to diagnose breast cancer, the training dataset should include a diverse set of cases, including different types of tumors, different stages, and patients with different characteristics (e.g., age, race, and ethnicity). This will ensure that the AI model learns to recognize a broad range of features and characteristics that are relevant to accurate diagnosis, rather than just memorizing features that are specific to the cases in the training dataset. Another solution is to use transfer learning, which involves training an AI model on a large dataset in one domain and then fine-tuning it on a smaller dataset in another domain. For example, an AI model trained on a large dataset of X-ray images of the chest can be fine-tuned on a smaller dataset of chest CT scans. This can help the model learn to recognize relevant features in the new domain more quickly and accurately. In addition, techniques such as ensemble learning, where multiple models are combined to produce a single output, can also help.
Interpretability
Advanced techniques for visualizing and explaining the outputs of AI algorithms can include techniques such as saliency mapping, which highlights the parts of an image that were most influential in the algorithm’s decision-making process. Incorporating AI techniques into clinical workflows, such as providing real-time feedback and decision support, can enhance the interpretability of AI outputs.
Ethics and bias
The most frequent ethical problem is unfairness caused by bias in data sources.[33] Advanced solutions for addressing ethical and social considerations can include techniques such as fair representation learning, which aims to ensure that algorithms are trained on diverse and representative datasets. To address ethical difficulties in data, resource allocation and practices, ethicists must be included in the supervision of the entire AI process with full independence to the ethical committee.[34] In addition, techniques such as adversarial training, where models are trained to be robust to adversarial attacks that might attempt to introduce bias, can help to improve transparency in AI-based diagnostic tools.[35]
Hardware limitations
Some possible solutions to address hardware limitations include [Figure 3]:
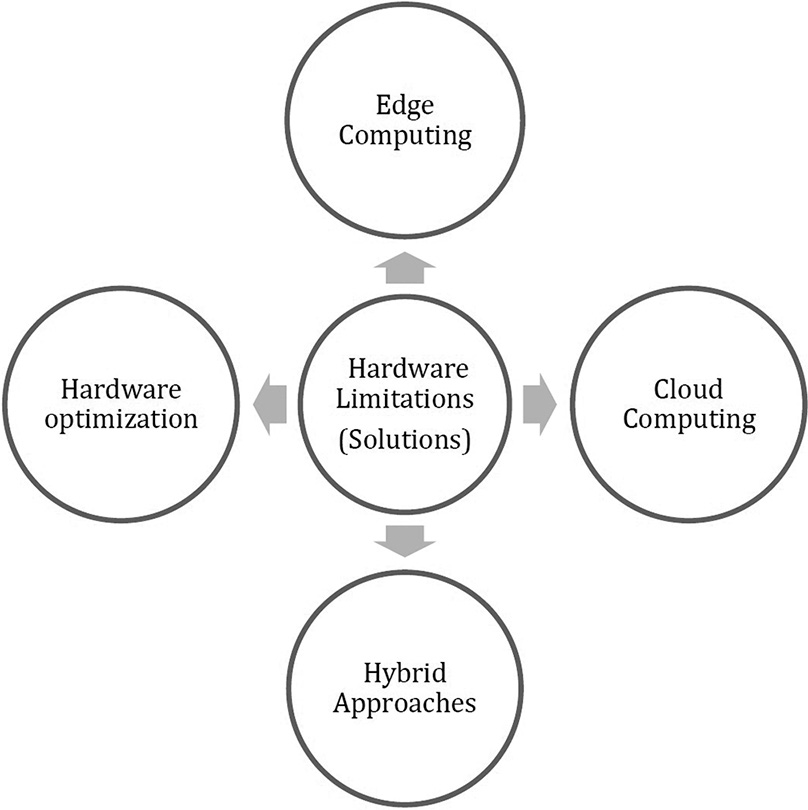
- Addressing solutions to hardware limitations faced by artificial intelligence.
Cloud computing
It allows medical institutions to outsource their computing needs to cloud-based infrastructure providers, which can offer significant scalability and performance improvements for AI-based medical imaging analysis. Cloud-based platforms such as Amazon Web Services or Google Cloud Platform can provide access to powerful graphics processing units (GPUs) and central processing units (CPUs) that can be used to train and validate AI models, without requiring significant investment.
Edge computing
It involves deploying AI algorithms on local devices, such as mobile phones or edge servers. It is useful for medical imaging applications where low latency and real-time analysis are critical, such as in emergency situations. It also reduces the risk of data breaches or other security issues.
Hardware optimization
Researchers have developed hardware-accelerated neural networks that can run on specialized hardware like field-programmable gate arrays or application-specific integrated circuits, which can offer significant performance improvements over traditional CPUs or GPUs.
Hybrid approaches
Hybrid approaches combine the benefits of cloud computing and edge computing, by using cloud-based infrastructure for training and validation, while deploying the resulting models on local devices for real-time analysis. This approach can offer the scalability and performance benefits of cloud computing, while also providing the low-latency and security benefits of edge computing.
The challenges and limitations of AI in pathology and radiology require advanced solutions that go beyond simple algorithmic improvements. It will be important for researchers and healthcare providers to work together to develop these solutions, with a focus on improving the accuracy, reliability and interpretability of AI-based diagnostic tools.
CONCLUSION
The development of AI in pathology and radiology has enormous potential to revolutionize how diseases are detected and treated, but it also presents several challenges that need to be addressed. These challenges include data quality, standardization, generalization, ethical considerations, and hardware limitations.
To overcome these challenges, researchers and clinicians need to work together to develop advanced solutions that take into account the unique characteristics of health-care data and the complex nature of diagnostic decision-making. Overall, AI has great potential to transform the way we diagnose and treat diseases, ultimately leading to better patient outcomes and a healthier society.
Declaration of patient consent
Patient’s consent not required as there are no patients in this study.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The author(s) confirms that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Artificial intelligence (AI) in medicine, current applications and future role with special emphasis on its potential and promise in pathology: Present and future impact, obstacles including costs and acceptance among pathologists, practical and philosophical considerations. A comprehensive review. Diagn Pathol. 2021;16:24.
- [CrossRef] [PubMed] [Google Scholar]
- Integrating pathology and radiology disciplines: An emerging opportunity? BMC Med. 2012;10:100.
- [CrossRef] [PubMed] [Google Scholar]
- Integrated diagnosis (radiology, pathology and genetics): Early experience. Anal Real Acad Nacl Med. 2019;136:99.
- [CrossRef] [Google Scholar]
- US Department of Health and Human Services: The Importance of Radiology and Pathology Communication in the Diagnosis and Staging of Cancer: Mammography as a Case Study. Washington, DC: Office of the Assistant Secretary for Planning and Evaluation; 2010.
- [Google Scholar]
- The artificial intelligence in digital radiology: Part 1: The challenges, acceptance and consensus. Healthcare (Basel). 2022;10:509.
- [CrossRef] [PubMed] [Google Scholar]
- The artificial intelligence in digital pathology and digital radiology: Where are we? Healthcare (Basel). 2021;9:30.
- [CrossRef] [PubMed] [Google Scholar]
- Artificial intelligence, radiology, and the way forward. Can Assoc Radiol J. 2019;70:10-2.
- [CrossRef] [PubMed] [Google Scholar]
- What the radiologist should know about artificial intelligence-an ESR white paper. Insights Imaging. 2019;10:44.
- [CrossRef] [PubMed] [Google Scholar]
- Enterprise implementation of digital pathology: Feasibility, challenges, and opportunities. J Digit Imaging. 2017;30:555-60.
- [CrossRef] [PubMed] [Google Scholar]
- Separating hope from hype: Artificial intelligence pitfalls and challenges in radiology. Radiol Clin. 2021;59:1063-74.
- [CrossRef] [PubMed] [Google Scholar]
- Available from: https://blog.mastek.com/how-ai-in-radiology-can-help-transform-processes-in-healthcare [Last accessed on 2022 Aug 22]
- The impact of artificial intelligence on radiography as a profession: A narrative review. J Med Imaging Radiat Sci. 2023;54:162-6.
- [CrossRef] [PubMed] [Google Scholar]
- Available from: https://intellipaat.com/blog/artificial-intelligence-in-healthcare [Last accessed on 2023 Jun 13]
- Deep learning nuclei detection in digitized histology images by superpixels. J Pathol Inform. 2018;9:5.
- [CrossRef] [PubMed] [Google Scholar]
- Computer-Aided Gleason Grading of Prostate Cancer Histopathological Images using TEXTON Forests In: Proceedings. IEEE International Symposium on Biomedical Imaging: From Nano to Macro. 2010. p. :636-9.
- [CrossRef] [PubMed] [Google Scholar]
- Image analysis with deep learning to predict breast cancer grade, ER status, histologic subtype, and intrinsic subtype. NPJ Breast Cancer. 2018;4:30.
- [CrossRef] [PubMed] [Google Scholar]
- Clinical-grade computational pathology using weakly supervised deep learning on whole slide images. Nat Med. 2019;25:1301-9.
- [CrossRef] [PubMed] [Google Scholar]
- Deep learning for classification of colorectal polyps on whole-slide images. J Pathol Inform. 2017;8:30.
- [CrossRef] [PubMed] [Google Scholar]
- Deep learning-based survival prediction for multiple cancer types using histopathology images. PLoS One. 2020;15:e0233678.
- [CrossRef] [PubMed] [Google Scholar]
- Whole-slide image focus quality: Automatic assessment and impact on AI cancer detection. J Pathol Informat. 2019;10:39.
- [CrossRef] [PubMed] [Google Scholar]
- Development and Validation of Machine Learning Based Natural Language Classifiers to Automatically Assign MRI Abdomen/Pelvis Protocols from Free-Text Clinical Indications. Society of Imaging Informatics in Medicine In: Annual Meeting. 2017.
- [Google Scholar]
- A review of computational methods for cervical cells segmentation and abnormality classification. Int J Mol Sci. 2019;20:5114.
- [CrossRef] [PubMed] [Google Scholar]
- Challenges related to artificial intelligence research in medical imaging and the importance of image analysis competitions. Radiol Artif Intell. 2019;1:e180031.
- [CrossRef] [PubMed] [Google Scholar]
- How much data is needed to train a medical image deep learning system to achieve necessary high accuracy?
- [Google Scholar]
- Artificial intelligence and machine learning in radiology: Opportunities, challenges, pitfalls, and criteria for success. J Am Coll Radiol. 2018;15:504-8.
- [CrossRef] [PubMed] [Google Scholar]
- Artificial intelligence and algorithmic bias: Implications for health systems. J Glob Health. 2019;9:10318.
- [CrossRef] [PubMed] [Google Scholar]
- Current applications and challenges of artificial intelligence in pathology. Hum Pathol Rep. 2022;27:300596.
- [CrossRef] [Google Scholar]
- Artificial intelligence and computational pathology. Lab Investig. 2021;101:412-22.
- [CrossRef] [PubMed] [Google Scholar]
- FAIR Data Principles. Available from: https://www.force11.org/group/fairgroup/fairprinciples [Last accessed on 2020 Jan 31]
- [Google Scholar]
- FAIR data sharing: The roles of common data elements and harmonization. J Biomed Inform. 2020;107:103421.
- [CrossRef] [PubMed] [Google Scholar]
- Artificial intelligence in pathology. Dtsch Ärztebl Int. 2021;118:199-204.
- [CrossRef] [PubMed] [Google Scholar]
- Implementing the DICOM standard for digital pathology. J Pathol Inform. 2018;9:37.
- [CrossRef] [PubMed] [Google Scholar]
- Opportunities and challenges of artificial intelligence in the medical field: Current application, emerging problems, and problem-solving strategies. J Int Med Res. 2021;49:3.
- [CrossRef] [PubMed] [Google Scholar]
- International AI ethics panel must be independent. Nature. 2019;572:415.
- [CrossRef] [PubMed] [Google Scholar]
- Generative Adversarial Nets. Advances in Neural Information Processing Systems In: NeurIPS Proceedings. 2014. p. :27.
- [Google Scholar]







