Translate this page into:
Symmetrical peripheral gangrene in a chronic kidney disease patient on hemodialysis
*Corresponding author: Gomathy Sankaranarayanan, Department of Nephrology, Government TD Medical College, Alappuzha, Kerala, India. komysankaran@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Karat A, Sankaranarayanan G, Maniyeri P, Sreeraj P, Balachandran P, Ananthamangalath S, et al. Symmetrical peripheral gangrene in a chronic kidney disease patient on hemodialysis. Indian J Med Sci 2022;74:157-8.
Abstract
Symmetrical peripheral gangrene (SPG) is a rare but well-described condition characterized by ischemic changes in the distal limbs with preserved flow in the major vessels. It results from thrombosis of the microcirculation resulting from a complex interplay of infectious and non-infectious factors. Often described as a complication of disseminated intravascular coagulation (DIC), it has got multiple aggravating factors. Timely recognition and management is important as significant residual disability is noted in surviving patients. Here, we describe a patient with chronic kidney disease on maintenance hemodialysis presenting with SPG associated with spontaneous bacterial peritonitis and DIC. She had multiple aggravating factors such as hypotension, use of inotropes, and renal failure. As there were no evidence-based guidelines and since the general condition of the patient was poor, she was managed with supportive care.
Keywords
Symmetrical peripheral gangrene
Disseminated intravascular coagulation
Microcirculation
Renal failure
Hemodialysis
INTRODUCTION
Symmetrical peripheral gangrene (SPG) refers to ischemic lesions affecting the distal extremities in the absence of occlusive diseases of major vessels supplying the limb. This rare condition was first described by Hutchinson in the year 1891 in a patient with shock. It carries significant morbidity and mortality and more than half of the patients ultimately require amputation of the limb. There is a scarcity of data regarding its incidence, etiology, prevention, and management as the condition is uncommon and very often underreported.
CASE REPORT
Our patient is a 53-year-old lady with chronic kidney disease undergoing regular thrice weekly hemodialysis for the past 4 years in our hospital. Her native kidney disease was biopsy-proven focal segmental glomerulosclerosis (FSGS) which was diagnosed 5 years back when she presented with impaired renal function test and subnephrotic range proteinuria and hypertension. Workup for secondary causes of FSGS was negative. She had no thrombotic complications in the past. Her disease progressed to dialysis-dependent stage after 1 year of detection and hemodialysis was initiated through the left brachiocephalic fistula as the vascular access.
On presentation to the hospital for routine dialysis, she complained of abdominal pain and low-grade fever for 2 days. It was a vague, dull aching, non-colicky, diffuse pain with no relation to food intake, and not associated with nausea, vomiting, altered bowel habits, or dysuria. On examination, she was conscious, oriented, pulse rate – 86/ min, respiratory rate – 16/min, temperature – 99.5°F, and BP – 140/90 mmHg. She weighed 65 Kg and her interdialytic weight gain was 1.7 Kg. She was pale. There were no icterus, cyanosis, clubbing, lymphadenopathy, or pedal edema. Abdomen palpation showed no tenderness, rigidity, or guarding. The presence of free fluid was indicated by positive shifting dullness. No organomegaly was noted. Examination of the other system was unremarkable. Vascular access site was clean and showed systolo diastolic bruit on auscultation.
After giving supportive treatment, hemodialysis was initiated. The patient developed chills and rigor 1 h after starting dialysis. She was found to have cold extremities and her blood pressure (BP) dropped to 80/50 mmHg. Resuscitated with bolus normal saline followed by noradrenaline infusion and dialysis was temporarily withheld. Antihistamine and steroid injections were administered. Since the BP remained low despite giving high doses of inotropes, dialysis was abandoned and she was shifted to the intensive care unit (ICU). Meanwhile, her investigation report showed features of spontaneous bacterial peritonitis (SBP) with disseminated intravascular coagulation (DIC).
The patient was started on broad-spectrum antibiotics and supportive care including inotropes and hemodialysis (sustained low-efficiency dialysis). BP improved and inotropes were stopped 48 h after ICU stay. On the 3rd day, she developed cyanotic changes involving the toes of both lower limbs and multiple blackish rashes over the upper limbs [Figures 1 and 2]. Peripheral pulses were well felt and the Doppler study of limbs showed a normal flow pattern. The echocardiogram did not show evidence of vegetation and blood culture was sterile. Cyanotic changes in the toes progressed and well-demarcated gangrene appeared. Surgery consultation was taken and advised to continue conservative management. Despite giving necessary supportive care, her general condition remained poor although she became hemodynamically stable. Hence, relatives opted for palliative care and she was transferred to a local nursing home.
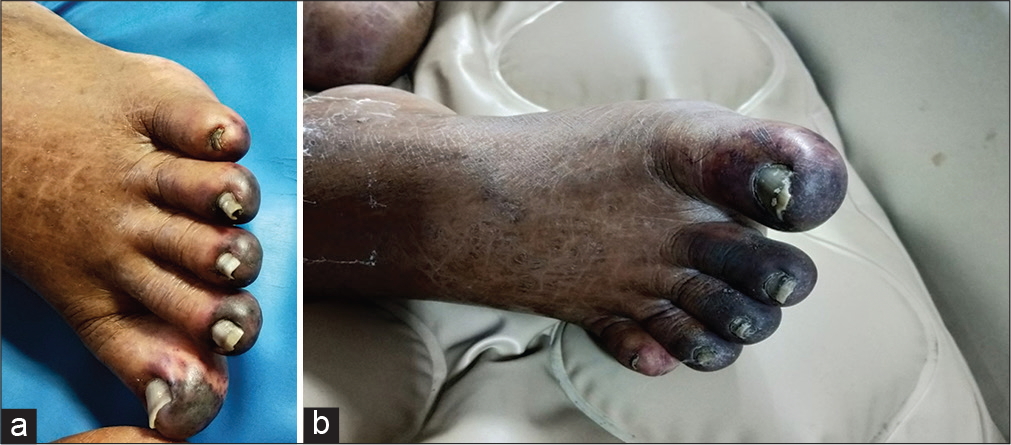
- (a) Gangrenous change involving left toes and (b) gangrenous change in the right toes.
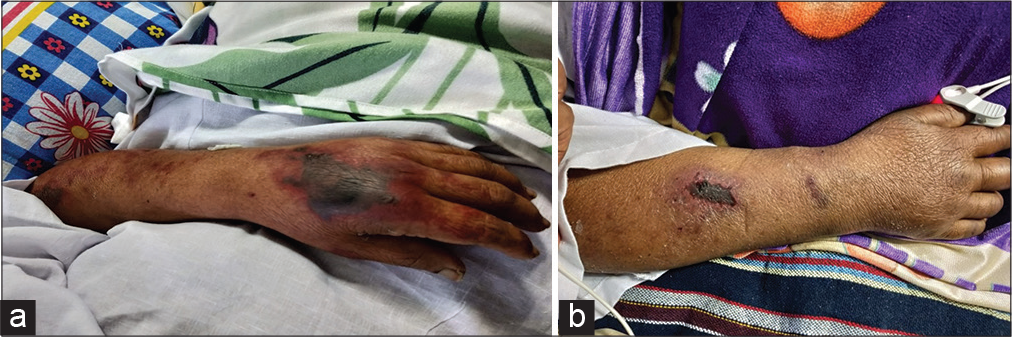
- (a) Gangrenous change in the dorsum of the left hand and (b) gangrenous change in the right hand.
DISCUSSION
SPG is a rare clinical manifestation of microcirculatory failure seen mostly in patients with DIC and conditions associated with low-flow states. It is considered as a cutaneous marker of DIC similar to purpura fulminans. There is an activation of the procoagulant pathway and inhibition of the anticoagulant and fibrinolytic system, leading to microvascular thrombosis. Cytokines such as IL1 and IL6 play a major role.[1] Thus, SPG encompasses the triad of circulatory shock, DIC, and natural anticoagulant depletion.[2] There are numerous etiologies for SPG including infective and non-infective causes. There are several aggravating factors for SPG such as asplenia, immunosuppression, diabetes mellitus, renal failure, cold injury, and use of vasopressors. Our patient had multiple risk factors, namely, sepsis, DIC, hypotension, use of inotropes, and chronic kidney disease. The probable focus of infection in this patient is SBP. We could not find any similar report of SBP, leading to SPG in the literature.
Management should focus on the timely treatment of the underlying etiologies and aggravating factors. Numerous specific treatment options for SPG were reported but none of them were supported by quality evidence. Eventually, amputation may be required in many cases but the procedure is deferred until the general condition of the patient improves and a clear line of demarcation develops.[3]
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Financial support and sponsorship
Nil.
References
- Bilateral endophthalmitis and symmetrical peripheral gangrene in a patient with chronic kidney disease on maintenance hemodialysis. Saudi J Kidney Dis Transpl. 2019;30:715-8.
- [CrossRef] [Google Scholar]
- Symmetrical peripheral gangrene in critical illness. Transfus Apher Sci. 2021;60:103094.
- [CrossRef] [PubMed] [Google Scholar]
- Symmetrical peripheral gangrene of bilateral feet and unilateral hand after administration of vasopressors during septic shock. BMJ Case Rep. 2018;2018:bcr2017223602.
- [CrossRef] [PubMed] [Google Scholar]






