Translate this page into:
Impact of COVID-19 on medical undergraduate students’ academics and its ramifications

*Corresponding author: Monica Gupta, Department of General Medicine, Government Medical College Hospital, Chandigarh, India. drmg1156@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Syal A, Arya Y, Gupta M. Impact of COVID-19 on medical undergraduate students’ academics and its ramifications. Indian J Med Sci 2021;73(1):26-9.
Abstract
Objectives:
COVID-19 pandemic has dramatically affected undergraduate medical education all over the world. This effect is most noteworthy on the medical students as clinical orientation and hands-on training are crucial toward development of basic medical skills. Various modifications to the methods of online teaching have been adopted in response to this pandemic to maintain continuity of medical education; however, we do not yet know the implications of this change.
Material and Methods:
To study the impact of this pandemic on medical students and to have a first-hand estimate of the adversities and challenges faced by them, an online questionnaire-based survey was conducted, administered through Google Forms maintaining anonymity. They were asked a series of multiple choice questions pertaining to the effects of this pandemic on their curriculum and academic activities. The responses received were analyzed by univariate analysis.
Results:
Almost half (46.4%) of students reported a decreased interest in medicine after suspension of hands on teaching/practical classes. A total of 136 respondents (69.38%) felt that they became less productive in studies during the pandemic. Approximately 74% respondents felt less motivated to study at home. More than two-thirds of the respondents felt that on graduation, their clinical skills will be inferior to the students who graduated during the “non-COVID” era. About 84.69% of students believed that their examinations should be postponed hoping to get appropriate clinical experience once things normalize.
Conclusion:
Majority of the students feel less motivated and less productive, amidst the transition. The major area that has been compromised is the clinical skills training, a crucial adjunct to theoretical teaching in medical schools, and almost all students believe that their clinical skills in the long term would remain inferior to those who graduated before this pandemic.
Keywords
COVID-19
Pandemic
Undergraduate
Medical students
Medical education
INTRODUCTION
Severe acute respiratory syndrome coronavirus 2 infection or COVID-19, as it is popularly known, is a novel strain of coronavirus that was declared as a pandemic by the WHO on March 11, 2020. This pandemic has resulted in a multitude of changes in our everyday lives. From lockdowns to social distancing and mandatory face coverings, this pandemic is rapidly changing the definition of “new normal.” The impact of this pandemic has been most noteworthy on “medical education,” as patient exposure, history taking and examination, and hands-on training are crucial toward development of basic medical skills, which medical students are gradually taught throughout the four professionals. The pandemic has led to major changes in the established curriculum. From online classes to suspension of clinical skills teaching and postponement of examinations, medical undergraduate education has suffered significantly. This is largely due to the unique challenges medical undergraduate education faces in terms of patient interaction, hospital visits, and case presentations.
To uncover the factors affecting medical education during the pandemic from medical students’ point of view, a questionnaire-based study was conducted. Although studies like this have been conducted in different regions of the world by Choi et al., Suzanne et al., Torda et al., Khalil et al., and Kapila et al., literature from the Indian subcontinent is lacking.[1-5] This makes our study unique and represents the views of students studying in all the four professionals, thereby providing insight into the adversities faced by them, which, in turn, can suggest necessary reforms that need to be instituted, to maintain the continuity of medical education, amidst these uncertain times.
MATERIAL AND METHODS
An online questionnaire-based survey was mailed to undergraduate medical students enrolled in various professional phases at Government Medical College and Hospital, Chandigarh, India. The online survey was administered through Google Forms while maintaining anonymity to increase freedom and truthfulness of responses. The questionnaire included a series of multiple choice questions with both closed- and open-ended responses pertaining to the effects of COVID-19 pandemic on their curriculum and whether the shift from “hands-on” teaching to online classes has affected their interest in pursuing medicine in future. The results were analyzed by univariate analysis.
RESULTS
A total of 400 medical students were sent the online questionnaire by email, out of which 196 medical students (n = 196) responded. Eighty-four students were residing in hostels (42.85%) in the college campus, while the rest were day scholars. The distribution of respondents in the 1st, 2nd, 3rd, and 4th professional is 29.08% (57), 25.51% (50), 10.2% (20), and 35.2% (69), respectively.
Almost half (46.42%) of the students reported a decreased interest in medicine after suspension of hands-on teaching/ practical classes. Only 22.44% (44) of respondents found video lectures to be better than classroom teaching. Ninety-eight respondents (50%) felt that they were still acclimatizing to the new method of learning through online classes. Similarly, almost three-quarters of students felt that their motivation to study had decreased as their curriculum shifted from “in person” to “online.” Students’ responses regarding their interest in medicine after transition from practical classes to video lectures are illustrated in Figure 1.

- Representation of variation in interest in medical education.
A total of 136 respondents (69.38%) felt that they became less productive in studies during the pandemic. About 50.51% reported a decrease while 36.73% reported an increase in the time spent studying. A total of 169 (86.22%) respondents preferred studying alone by themselves, whereas 27 (13.77%) preferred studying in groups through video conferencing. A total of 111 respondents (56.63%) felt that tele-education is the new reality. Quite a good number (41.32%) of respondents felt that online teaching resulted in sparing of time that would otherwise be spent in commuting to college.
About 34.69% of students reported a decrease 33.7% an increase in their level of understanding of online lessons compared to contemporary classroom teaching and 31.63% felt that it was unchanged [Figure 2]. A total of 157 (80.10%) students positively responded that their teachers were able to clear their doubts through electronic means. Approximately half of the students believed that video conferencing would be the best method, followed by e-mails and tele-consultation, to clear doubts with their teachers.
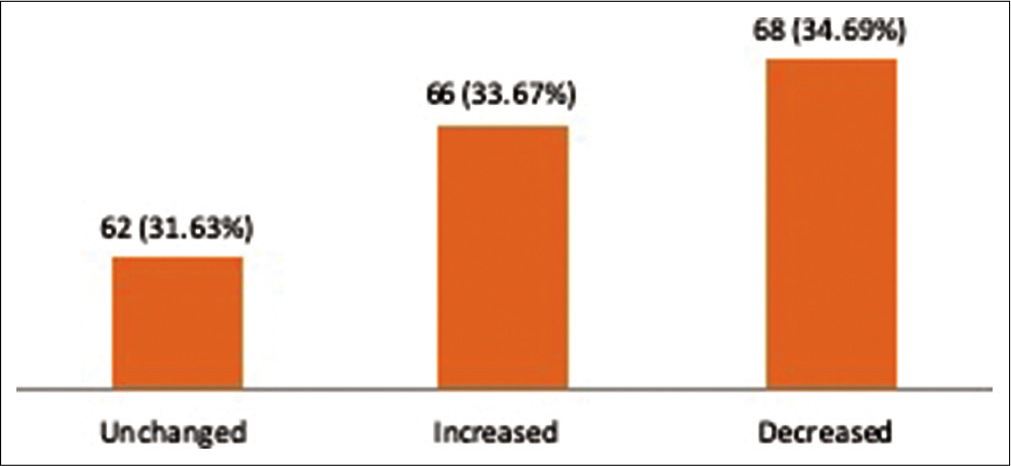
- Representation of understanding of medical subjects through tele-education.
Almost all respondents (192 of 196) believed that suspension of practical classes and hands on exposure in laboratories/ clinics and lack of in-person history taking and examination would affect their clinical knowledge and skills as a future physician. More than two-thirds of respondents felt that on graduation, their clinical skills will be inferior to the students who graduated during the “Non-COVID” era.
Although one-third of respondents felt that this pandemic had instilled fear in their minds with regard to pursuing medicine further, only a small percentage (15.3%) gave a reasonable consideration (>5 points on scale) to the idea of dropping out of medical school. These data were acquired through rating on a 10-point numerical scale (with 1 being “did not consider” and 10 being “strongly considered”).
About 73% of students felt that their examinations should be simplified or made easier than before. About 70.4% responded that the examinations should be conducted in their medical schools with all due precautions instead of video conferencing. Finally, a majority (82.65%, 162 respondents) of the students responded that they would prefer their examinations being postponed, so as to get adequate clinical experience once things normalize.
DISCUSSION
The impact of COVID-19 on medical education is unprecedented. Students are facing numerous distinctive challenges in these uncertain times. Medical education is largely patient centered. The understandable lack of patient interaction, due to the unprecedented yet necessary measures of containment, has added to the students’ disadvantage. The replacement of in-person classes with online lectures is a crucial step in the current situation, however, the students are at a loss of clinical encounters. Students currently enrolled in MBBS training are not acclimatized to the new and crucial changes in the hospital settings and might be too amateur to understand the hazards of exposure and the protocols instituted in hospitals amidst the pandemic. In-person and clinical classes have been suspended in totality, in most parts of the world. In response to this, online lectures, and case simulations through video conferencing, tele-lectures, webinars, with the help of various tools such as Zoom, Google Meet, Skype, Go to Webinars, and other platforms are being conducted. Our study highlights the cardinal problems faced by medical students in all four professional years, in a prestigious medical institute of North India. Similar questionnaire-based surveys are being conducted in India, in the wake of this pandemic, pertaining to both undergraduate[6-9] and postgraduate[10] medical students. Several key issues were addressed in our study. Half of the students reported that they were still acclimatizing to this change. Many now believe that tele-education is the new reality. In our study, where a majority of the students felt that they were less productive and less motivated to study. Almost all the students felt that their clinical skills would suffer, due to a lack of clinical exposure. On the other hand, 36.73% reported an increase in the number of hours spent studying. Many students reported a decreased interest in medicine due to a switch to online classes. This is due to the necessary omission of hospital visits and clinical classes and accompanied by a decreased understanding of the subjects through online classes, as reported by a majority of the students, although teachers were adequately able to clear their doubts through electronic means. These changes have created a sense of fear and anxiety among these budding doctors, adding to their apprehension, and in turn affecting their studies.
The major impact of this “lack of patient interaction” has undoubtedly been on final year medical students.[11] In our study, many students reported that they would be more comfortable if the examinations were delayed so that they could get appropriate clinical experience once the pandemic settles. Our study was limited by the inclusion of only a single institute, although the sample size was fair.
CONCLUSION
The impact of COVID-19 pandemic on medical students is significant. Students feel anxious and uncertain about the current situation and the future of medical education. Various modifications to the methods of online teaching have been adopted to maintain continuity of medical education. This impact has been tremendous due to suspension of hands-on training and patient interaction, crucial adjuncts to “holistic teaching” in medical schools. A significant majority of students feel that this would have lasting impact on their skills as a future physician. Although online teaching has caught up with theoretical in-person teaching, and most students are also able to communicate and clarify their doubts with their teachers, the deficiency of clinical classes cannot be overlooked and compensated by any means.
Declaration of patient consent
Patient’s consent not required as there are no patients in this study.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- The impact of the COVID-19 pandemic on final year medical students in the United Kingdom: A national survey. BMC Med Educ. 2020;20:206.
- [CrossRef] [PubMed] [Google Scholar]
- Medical student education in the time of COVID-19. JAMA. 2020;323:2131-2.
- [CrossRef] [PubMed] [Google Scholar]
- The impact of the COVID-19 pandemic on medical education. Med J Aust. 2020;213:334e1.
- [CrossRef] [PubMed] [Google Scholar]
- The sudden transition to synchronized online learning during the COVID-19 pandemic in Saudi Arabia: A qualitative study exploring medical students' perspectives. BMC Med Educ. 2020;20:285.
- [CrossRef] [PubMed] [Google Scholar]
- The importance of medical student perspectives on the impact of COVID-19. Br J Surg 2020
- [CrossRef] [PubMed] [Google Scholar]
- Perception and attitudes versus medical writing skills. South Asian J Cancer. 2015;4:55-7.
- [CrossRef] [PubMed] [Google Scholar]
- Assessment of online teaching as an adjunct to medical education in the backdrop of COVID-19 lockdown in a developing country-an online survey. Indian J Ophthalmol. 2020;68:2399-403.
- [CrossRef] [PubMed] [Google Scholar]
- Knowledge and perceptions about COVID-19 among the medical and allied health science students in India: An online cross-sectional survey. Clin Epidemiol Glob Health 2020
- [CrossRef] [PubMed] [Google Scholar]
- Anxiety, depression and behavioural changes in junior doctors and medical students associated with the Coronavirus pandemic: A cross-sectional survey. J Obstet Gynaecol India. 2020;1:1-5.
- [CrossRef] [Google Scholar]
- Impact of COVID-19 on post-graduate orthopaedic training in Delhi-NCR. J Clin Orthop Trauma. 2020;11(Suppl 5):S687-95.
- [CrossRef] [PubMed] [Google Scholar]






